Tracheotomy vs Tracheostomy: Essential Differences Explained
When it comes to life-saving airway procedures, tracheotomy and tracheostomy are terms that often cause confusion, even among healthcare professionals. While closely related, these procedures serve distinct purposes in respiratory management. Many people mistakenly use these terms interchangeably, but understanding their differences is crucial for patients, caregivers, and medical professionals alike. Have you ever wondered what exactly happens during these procedures and why they're performed?
For individuals facing respiratory distress or those caring for someone with airway issues, grasping the nuances between these procedures can provide clarity during challenging medical situations. This comprehensive guide breaks down everything you need to know about tracheotomy versus tracheostomy, from basic definitions to recovery expectations and long-term management.
What is a Tracheotomy?
A tracheotomy is specifically the surgical incision or creation of an opening into the trachea (windpipe) through the neck. This procedure involves making a precise cut on the anterior (front) part of the neck to establish a direct airway through an incision made on the trachea. Think of it as the initial "doorway" created to access the airway.
During a tracheotomy, surgeons carefully navigate through several layers of tissue, including skin, subcutaneous fat, and muscle, before reaching the trachea itself. Using specialized surgical instruments, they create a controlled opening between the tracheal rings, which are the C-shaped cartilage structures that give the windpipe its shape and stability. This opening serves as the entry point for a breathing tube if one is to be inserted.
It's important to understand that a tracheotomy can be performed in different settings depending on the urgency of the situation. In emergency scenarios where a patient's airway is suddenly compromised—perhaps due to severe facial trauma or an allergic reaction—an emergency tracheotomy might be performed at the bedside or even in the field. In contrast, planned tracheotomies typically take place in operating rooms under more controlled conditions.
The tracheotomy procedure itself is just the first step in airway management. Once completed, the surgeon has created a pathway to the airway, but depending on the patient's needs, this may or may not be followed by the insertion of a tube. In some cases, a temporary tracheotomy might be performed to remove an obstruction or foreign body, after which the opening can be allowed to heal without long-term tube placement.
What is a Tracheostomy?
While a tracheotomy refers to the creation of the opening, a tracheostomy involves the complete procedure of not only making the incision but also inserting and maintaining a tube through this opening. The tracheostomy tube serves as a direct pathway for air to enter the lungs, bypassing the upper airway structures like the nose, mouth, and throat.
These tubes are carefully designed medical devices that come in various sizes and types to meet different patient needs. A standard tracheostomy tube consists of an outer cannula that remains in place, an inner cannula that can be removed for cleaning, and sometimes a cuff at the distal end that can be inflated to create a seal within the trachea. This seal is particularly important when the patient requires mechanical ventilation, as it prevents air from escaping around the tube.
Once in place, a tracheostomy tube can serve multiple purposes. It can be connected to a mechanical ventilator to provide breathing support, used to deliver supplemental oxygen, or simply maintain a patent airway in patients who cannot maintain their own. Additionally, the tube provides convenient access for suctioning secretions from the lungs, which is especially valuable for patients who have difficulty clearing their own airways due to weakness or neurological conditions.
Unlike the tracheotomy procedure itself, which is completed in minutes to hours, a tracheostomy refers to the ongoing presence and management of the tube and stoma (opening). This can last for days, weeks, months, or even become a permanent arrangement depending on the underlying medical condition. For some patients with chronic respiratory failure or severe neurological impairments affecting breathing, a tracheostomy may become a life-long necessity.
Key Differences Between Tracheotomy and Tracheostomy
Understanding the distinction between these two terms is more than just a matter of medical semantics—it reflects important differences in both procedure and patient management. Let me break down the key differences in detail:
| Aspect | Tracheotomy | Tracheostomy |
|---|---|---|
| Definition | The surgical procedure of creating an incision in the trachea | The complete process including the insertion and maintenance of a tube through the incision |
| Primary Purpose | Creating access to the airway | Establishing a stable, long-term artificial airway |
| Duration | Refers to the surgical procedure only (minutes to hours) | Can be temporary or permanent (days to lifetime) |
| Equipment | Surgical instruments for creating the opening | Includes the tracheostomy tube and maintenance supplies |
| Patient Care Requirements | Immediate post-surgical wound care | Ongoing stoma care, tube maintenance, suctioning, and monitoring |
| Complications | Primarily surgical complications (bleeding, infection) | Both surgical and long-term complications (tube obstruction, granulation tissue, tracheal stenosis) |
| Reversibility | The incision can heal if no tube is placed | Removal of the tube may allow stoma closure, though some patients require surgical closure |
| Common Settings | Operating room or emergency setting | Intensive care units, long-term care facilities, or home care |
Medical Indications for Tracheotomy and Tracheostomy
Healthcare providers may recommend these procedures for various medical conditions. Understanding when and why they're necessary can help patients and families prepare for what to expect. The decision to perform a tracheotomy or tracheostomy is never taken lightly and typically occurs after careful consideration of the patient's condition and prognosis.
The most common indications for these procedures include:
- Upper airway obstruction: This can result from foreign bodies lodged in the airway, tumors, trauma, infections causing severe swelling, or congenital abnormalities that narrow the airway passage.
- Need for prolonged mechanical ventilation: Patients who require breathing support for extended periods often benefit from tracheostomy over continued endotracheal intubation, as it's more comfortable and reduces sedation requirements.
- Neurological conditions: Disorders affecting the brain, spinal cord, or nerves can impair a person's ability to protect their airway or clear secretions, necessitating tracheostomy for airway management and pulmonary toilet.
- Severe sleep apnea: In rare cases where conventional treatments like CPAP machines or less invasive surgeries fail, tracheostomy may be considered as a treatment option.
- Facial trauma or burns: Extensive injuries to the face may distort normal anatomy and compromise the airway, requiring a surgical airway below the level of injury.
- Congenital defects: Conditions present at birth such as laryngeal hypoplasia (underdeveloped voice box) or vascular webbing that obstructs breathing.
Emergency versus planned procedures also differ significantly in their approach and execution. Emergency tracheotomies are performed when there's an immediate threat to life due to acute airway compromise. These procedures may be done with limited resources and under less-than-ideal conditions. In contrast, planned procedures allow for comprehensive patient preparation, optimal surgical conditions, and detailed discussions about post-procedure care and expectations.
The Tracheostomy Procedure: What to Expect
For patients and families facing a planned tracheostomy, knowing what to expect can help alleviate anxiety and prepare for recovery. The procedure typically follows these steps:
- Pre-operative preparation: The patient receives general anesthesia for a planned procedure, though emergency cases may use local anesthetics. The neck is positioned to optimize access to the trachea, usually with a small cushion placed under the shoulders to extend the neck slightly.
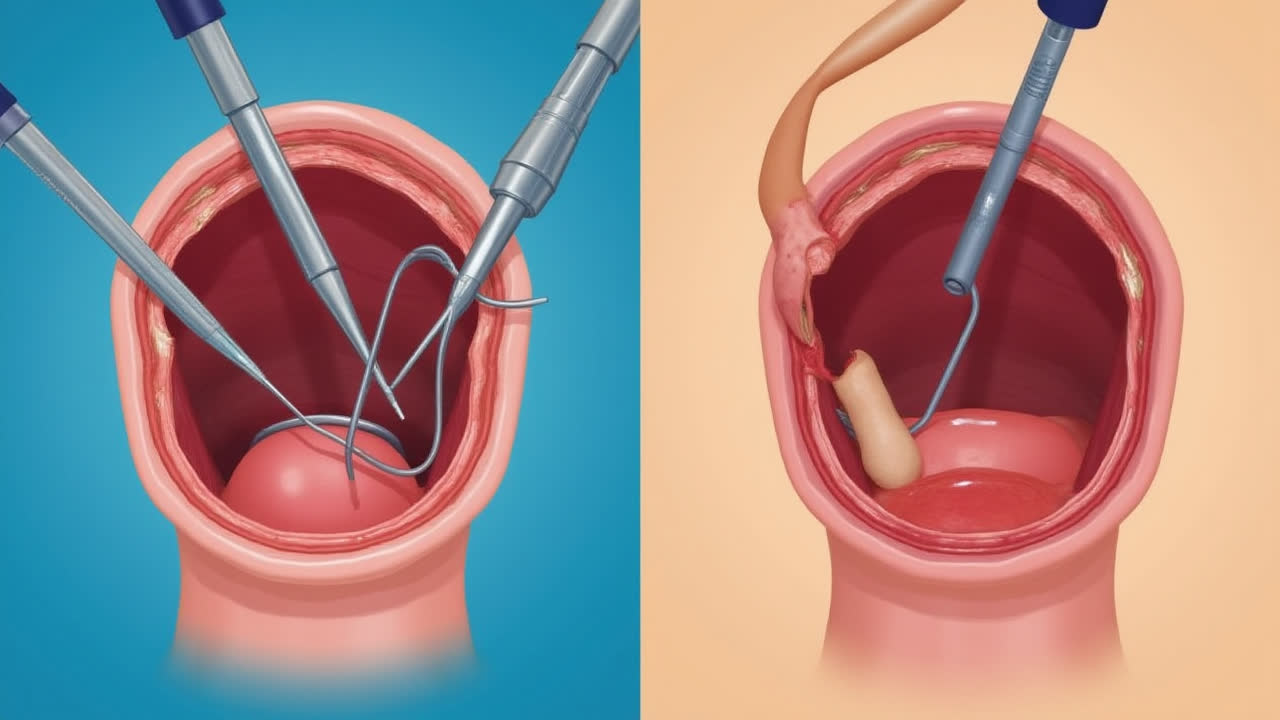
- Surgical approach: After sterilizing the skin, the surgeon makes a horizontal incision in the lower part of the neck. Layers of tissue are carefully separated to expose the trachea, with special attention paid to avoiding blood vessels and the thyroid gland.
- Tracheal incision: Once the trachea is exposed, an incision is made between the tracheal rings, typically between the second and third or third and fourth rings. This creates the opening (tracheotomy) through which the tube will be inserted.
- Tube placement: The appropriate size tracheostomy tube is selected and inserted into the opening. The tube is secured in place with tracheostomy ties or sutures to prevent accidental displacement.
- Confirmation and completion: Proper tube placement is confirmed through various methods, including direct visualization, ease of air movement, and sometimes imaging. The surgical site is cleaned, and dressings are applied as needed.
I've seen many patients surprised by how quickly they adapt to breathing through a tracheostomy tube. Initially, it may feel strange and uncomfortable, but the body generally adjusts within days. One important thing to remember is that patients with a new tracheostomy typically cannot speak immediately after the procedure, as air no longer passes through the vocal cords during breathing. Communication boards, writing tools, or specialized speaking valves may be used to help patients express themselves until they adjust or learn alternative communication methods.
Recovery time varies widely depending on the reason for the procedure and the patient's overall health. Some patients may require intensive care monitoring for several days, while others might recover more quickly. Regardless of the setting, specialized care of the tracheostomy site is essential to prevent complications and promote healing.
Potential Complications and Management
Like any surgical procedure, both tracheotomy and tracheostomy carry certain risks and potential complications. Being aware of these can help patients and caregivers recognize warning signs early and seek appropriate medical attention. Some common complications include:
- Bleeding: This can occur during the procedure or in the days following, particularly if blood vessels in the neck are damaged.
- Infection: The stoma (opening) can become infected, leading to redness, swelling, pain, and discharge. Proper stoma care and hygiene are essential for prevention.
- Tube displacement or obstruction: The tracheostomy tube can become dislodged or blocked by secretions, causing respiratory distress. Caregivers should learn proper suctioning techniques and emergency protocols.
- Tracheal stenosis: Narrowing of the trachea can develop as a long-term complication, especially in patients with prolonged tracheostomy.
- Granulation tissue: Excessive tissue growth around the stoma can cause bleeding and difficulty with tube changes.
- Tracheomalacia: Weakening of the tracheal walls can occur with long-term tube placement, causing the airway to collapse during breathing.
- Tracheoesophageal fistula: An abnormal connection between the trachea and esophagus can develop, allowing food or liquids to enter the lungs.
Management of these complications depends on their severity and may range from simple interventions like more frequent cleaning and suctioning to surgical repair for more serious issues. Regular assessment by healthcare professionals familiar with tracheostomy care is crucial for early detection and treatment of problems.
Living with a tracheostomy requires adaptation and learning new care routines. Patients and caregivers receive comprehensive training before discharge, covering topics such as stoma cleaning, tube care, suctioning techniques, and emergency measures. Support groups and home health services can provide additional assistance during the transition to home care.
Long-term Care and Quality of Life
For patients requiring long-term or permanent tracheostomy, adapting to life with the tube becomes an important focus. Many people lead full, active lives with a tracheostomy, though certain adjustments are necessary. Specialized covers can protect the stoma from dust, cold air, and small particles. Waterproof covers allow for showering, though swimming and submersion in water should generally be avoided.
Communication options have expanded significantly in recent years. Speaking valves like the Passy-Muir valve allow airflow through the vocal cords during exhalation, enabling speech. For patients unable to use speaking valves, alternatives include electrolarynx devices, text-to-speech applications, and communication boards.
The psychological impact of tracheostomy shouldn't be underestimated. Body image concerns, communication frustrations, and changes in social interactions can affect emotional well-being. Counseling and support groups specifically for tracheostomy patients can provide valuable emotional support and practical tips for coping with these challenges.
Regular follow-up with healthcare providers remains important even for stable, long-term tracheostomy patients. Periodic tube changes (typically every 4-12 weeks depending on the type), stoma assessment, and evaluation of whether the tracheostomy is still necessary are all part of ongoing care. For some patients, particularly those who had tracheostomies placed for temporary conditions, decannulation (removal of the tube) may eventually become possible as their condition improves.
Frequently Asked Questions About Tracheotomy and Tracheostomy
Can a person eat normally with a tracheostomy tube?
Many patients with tracheostomies can eat normally, especially if they have a cuffless tube or if the cuff is deflated during meals. However, swallowing may be affected in some patients due to the underlying condition or changes in neck anatomy. A speech-language pathologist typically evaluates swallowing function and may recommend texture modifications or swallowing strategies. For patients at high risk of aspiration, alternative feeding methods like feeding tubes might be necessary temporarily or permanently.
How long does recovery from a tracheostomy procedure take?
Initial recovery from the surgical procedure typically takes 1-2 weeks, during which time the stoma begins to mature and stabilize. However, adaptation to living with a tracheostomy is an ongoing process that varies widely among patients. Those with temporary tracheostomies may undergo a weaning process over weeks to months before the tube is removed. For patients with permanent tracheostomies, learning to manage daily care routines and adapting to communication changes may take several months. Full psychological adjustment often takes longer and is highly individual.
Will there be a visible scar after a tracheostomy tube is removed?
Yes, most patients will have some degree of scarring after a tracheostomy tube is removed. The appearance of the scar depends on several factors, including how long the tube was in place, individual healing characteristics, and whether surgical closure was required. Small stomas from short-term tracheostomies often close spontaneously, leaving a small, flat scar. Longer-term tracheostomies may require surgical closure and can result in more noticeable scarring. Scar management techniques, including silicone sheets, massage, and topical treatments, may help minimize the appearance of scars over time.
Conclusion
Understanding the differences between tracheotomy and tracheostomy is more than just a matter of medical terminology—it provides valuable insight into respiratory management for patients with airway challenges. While a tracheotomy refers specifically to the surgical creation of an opening in the trachea, a tracheostomy encompasses the entire process of establishing and maintaining an artificial airway through that opening.
For patients and families navigating decisions about these procedures, clear communication with healthcare providers is essential. Asking questions about the expected duration of tube placement, care requirements, and potential for eventual decannulation can help set realistic expectations and prepare for the road ahead.
Medical technology and techniques continue to evolve, with less invasive tracheostomy methods gaining popularity and improved tube designs enhancing comfort and function. As research advances, we can expect further improvements in both the procedures themselves and the quality of life for patients requiring these interventions.
Whether temporary or permanent, these airway management strategies have saved countless lives and improved breathing for many patients with complex medical conditions. With proper training, support, and follow-up care, individuals with tracheostomies can maintain good quality of life while managing their respiratory needs effectively.